Global Women's Health Academy

Regional Scientific Update Meeting Featuring Highlights from ESHRE 2016: Asia Pacific
THE REGIONAL SCIENTIFIC UPDATE MEETING FEATURING HIGHLIGHTS FROM ESHRE 2016:
ASIA PACIFIC MEETING SUMMARY
Saturday, September 17, 2016 | KUALA LUMPUR, MALAYSIA
This meeting was attended by 109 participants, from 10 countries. Lawrence Sherman, FACEHP, CHCP welcomed the participants and explained the rationale for the meeting and the scientific program. A key-pad survey was conducted to see the distribution of participants in this meeting.
Prof. PC Wong gave an introduction of the Global Fertility Academy and its activities so far, and what it hopes to achieve with a scientific meeting to share the highlights of the ESHRE 2016 Annual Meeting. The scientific program was divided into 6 parts.
1. INDIVIDUALISED IVF: INTRODUCTION TO THE POSEIDON CONCEPT
By Dr. Gavin Sacks
Differences between patients such as age, ovarian reserve, BMI can impact the success of IVF. IVF practice is currently extended to very diverse patient phenotypes and genotypes. Adapting the IVF procedure for each patient is crucial to optimise its efficacy and safety.
The POSEIDON Groupi suggested 4 groups of patients with different degree of low response.
- Group 1: Patients < 35 years with sufficient prestimulation ovarian reserve parameters (AFC ≥ 5, AMH ≥ 1.2ng/mL) and with an unexpected poor or suboptimal ovarian response. Subgroup 1A: < 4 oocytes Subgroup 1B: 4-9 oocytes
- Group 2: Patients ≥ 35 years with sufficient prestimulation ovarian reserve parameter (AFC ≥ 5, AMH ≥ 1.2 ng/mL) and with an unexpected poor or suboptimal ovarian response. Subgroup 2A: < 4 oocytes Subgroup 2B: 4-9 oocytes
- Group 3: Patients < 35 years with poor ovarian reserve prestimulation parameters (AFC < 5, AMH < 1.2 ng/mL)
- Group 4: Patients ≥ 35 years with poor ovarian reserve prestimulation parameters (AFC < 5, AMH < 1.2 ng/mL)

Based on above, there are 2 categories of patients with low responses.
The suboptimal response group where the retrieval of 4 to 9 oocytes at any given age with a significantly lower live birth rate compared with normal responders and the hyporesponse group where higher dosage of gonadotropins and a more prolonged stimulation are required to obtain an adequate number of oocytes.
The participants were enthused with this new concept by the POSEIDON Group. They agreed that in clinical practice the group of suboptimal response was not uncommon and this concept encouraged them to how best to treat them in subsequent cycles.
2. EMERGING VIEW TO MANAGING THE POOR-RESPONDER
By Dr. Xu Yang
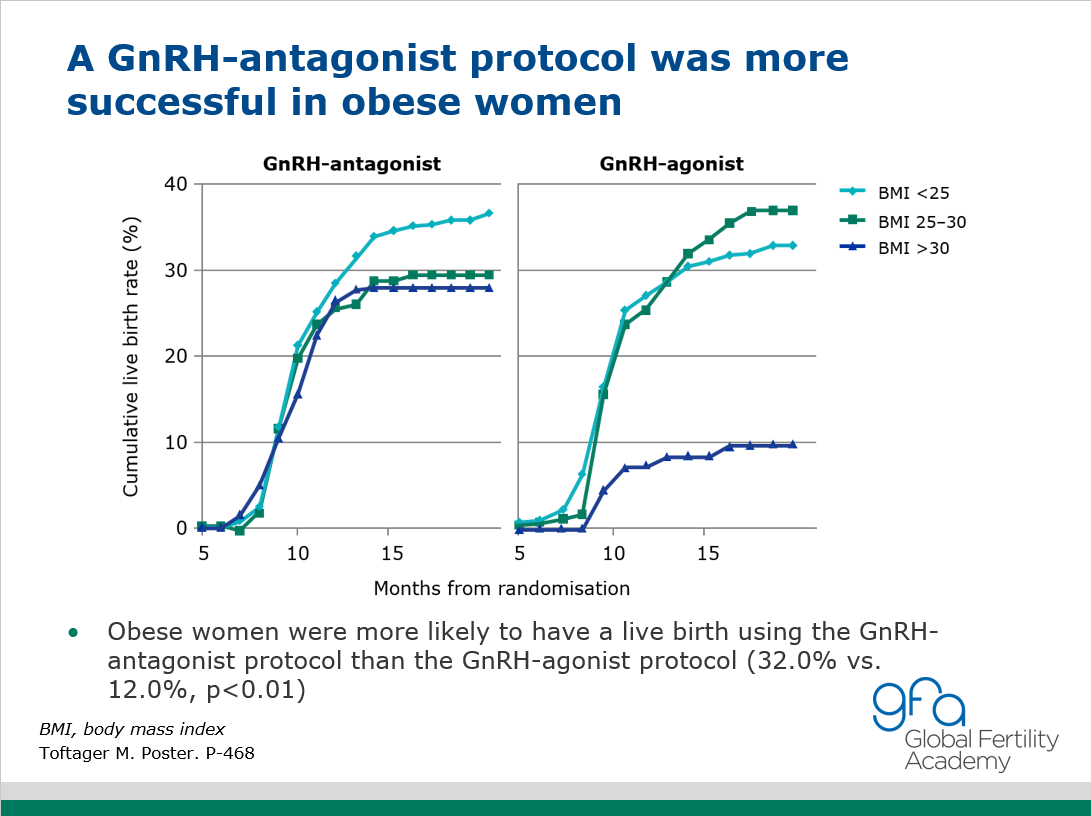
Cumulative live birth rates after one ART cycle including one subsequent frozen-thaw cycles in 1050 women in a RCT comparing GnRH-antagonist vs GnRH agonist protocol. (M Toftager) There was no difference in cumulative live birth rates between GnRH antagonist and GnRH agonist protocol groups. However, in obese patients, cumulative live birth rate was significantly higher in the GnRH-antagonist protocol group.
In a poster, YP Li showed that in poor responders, higher baseline estradiol levels may reflect earlier follicular recruitment in the late luteal phase leading to a short follicular phase. Shorter stimulation duration may reflect better granulosa cell function and may result in higher pregnancy rates. Prolonged stimulation duration could result in post mature oocyte in poor responders. In normal responders, shorter stimulation may not allow optimal oocyte maturation. Stimulation duration might be considered an adjunct parameter in determination of hCG timing in both poor and normal responders.
The discussion revolved around how best to manage the poor responders. There was no consensus as to the best protocol for the poor responders.
3. SPECIAL SITUATIONS: PCOS AND ENDOMETRIOSIS
By Prof. PC Wong
Y. Cheong’s oral presentation showed that women with endometriosis had a lower number of oocyte collected, but this did not affect the fertilization rate. There was a higher rate of early embryo arrest and this indicated perhaps a poor oocyte quality.
Sudiman’s poster showed that severe endometriosis decreased both the fertilization rate and the number of top quality embryo produced. This significantly decreased the clinical pregnancy rate in women with severe endometriosis undergoing ICSI.
The discussion that followed showed that many clinicians do not carry out laparoscopy routinely prior to embarking on IVF. There was also no consensus as to the benefits of treating minimal to mild endometriosis patients prior to IVF.
D. D. Wu’s poster presentation is a study of PCOS patients undergoing IVF. It showed that higher serum testosterone levels was detected on hCG trigger day in PCOS patient. The high testosterone levels may result in impaired endometrial receptivity leading to poor pregnancy outcomes in PCOS patients. While this was an interesting finding, the discussants felt that not enough is known i.e. what levels of testosterone are considered high, does that meant that if the testosterone levels are high then the patient should “freeze all” embryos, etc. Most agreed to watch this space.
4. APPROACHES TO HYPER-RESPONSIVENESS AND OHSS
By Prof. Shee-Uan Chen
Currently there are no accepted risk scores for OHSS. Shields and colleaguesii have developed a tool to assess for high risk OHSS. This risk score was calculated from two scores of age, maximum E2 and follicular count.
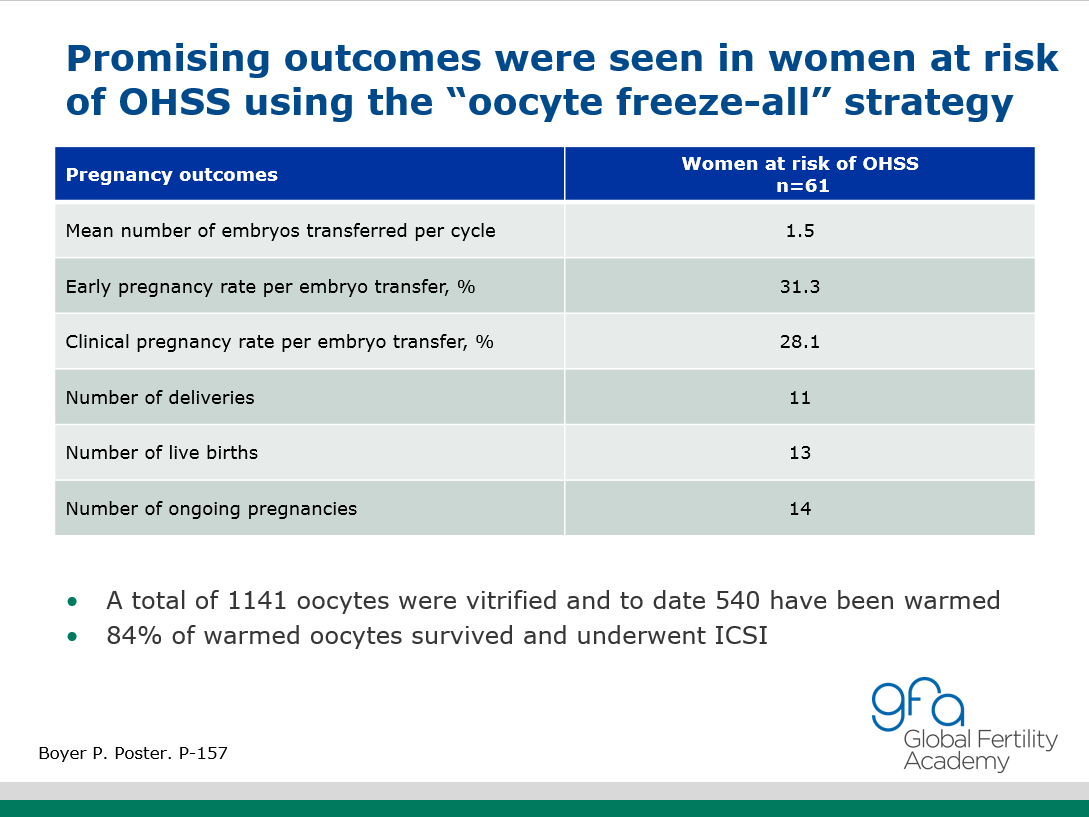
P. Boyer introduced the idea of freezing all oocytes in patients with high risk of OHSS. The preliminary results were encouraging. This is an alternative to the “freeze-all” strategy in patients who are adverse to embryo cryopreservation.
The participants acknowledged that “freeze all oocyte” is an alternative to “freeze all embryo” now that vitrification of eggs are quite successful.
5. LUTEAL PHASE SUPPORT
By Dr. Keiji Kuroda
Dr. Kuroda reviewed the physiology of implantation and decidualization of the endometrium. He also reviewed causes of luteal phase defect in ART treatment. Liu in a poster presentation showed that oocyte retrieval for the follicular and luteal phase in the same IVF cycle in patients with diminished ovarian reserve have comparable fertilization rates and form embryos with comparable cleavage and blastulation rates. Thus oocyte retrieval from both follicular and luteal phase by double stimulation protocol provide an approach for increasing oocyte retrieval per IVF cycle in patients with diminished ovarian reserve.
Generally the participants enjoyed the review of luteal phase support in IVF patients.
6. AMH AND BIOMARKERS OF IVF OUTCOME: HOW VALUABLE?
By Dr. Rohit Gutgutia
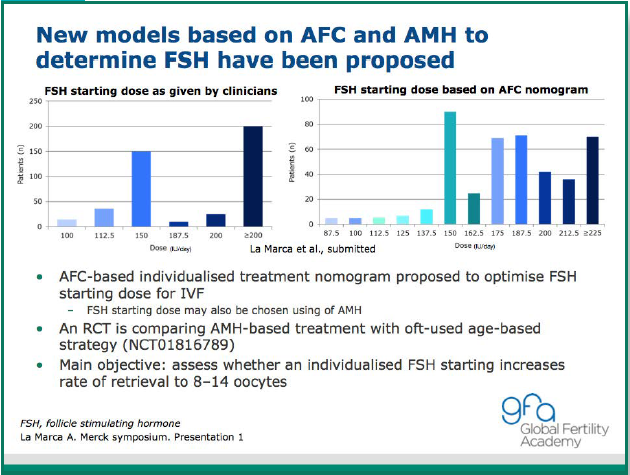
La Marca in an oral presentation suggested that one marker of ovarian response (either AMH or AFC) is adequate, but a combination of markers may improve diagnostic performance. Preliminary result show that models based on a combination of AMH and AFC may be clinically useful to determine the optimum FSH starting dose.
Marino’s poster presentation also suggested a normogram to be the basis for choosing the optimal starting dose of FSH.
By a quick show of hands, more participants used AFC than AMH as a test of ovarian reserve. The reason being that all the clinicians present had direct/easy access to transvaginal ultrasound scan while not all have a reliable/convenient AMH assay.
Of those who utilised both AMH and AFC, they tend to be guided by the AFC result when there was a divergent test result between AFC and AMH. This was attributed to the fact that clinicians trusted their own ultrasound scans more than the laboratory results.
After every two sections, there were time allocated to small group discussion followed by the faculty panel discussion. Many questions were raised in vital discussions. Many participants shared their personal experience and many queried how the meeting pointers could fit into their clinical practice.
Overall it was a very successful meeting. The feedback from the participants were very positive and everyone felt that the meeting was useful to them.
i POSEIDON GROUP, Alviggi, C., Andersen, C. Y., Buehler, K., Conforti, A., De Placido, G., ... & Sunkara, S. K. (2016). A new more detailed stratification of low responders to ovarian stimulation: from a poor ovarian response to a low prognosis concept. Fertility and sterility. 2016, 105:6. 1452-1453
ii Shields, R., Vollenhoven, B., Ahuja, K. and Talmor, A. (2016), Ovarian hyperstimulation syndrome: A case control study investigating risk factors. Aust N Z J Obstet Gynaecol. doi:10.1111/ajo.12515
ESHRE SESSIONS: POSTERS, ORALS AND SUPPORTING STUDIES
Individualising IVF: Introduction to the POSEIDON Concept
How to better characterize the poor ovarian response spectrum to maximize treatment outcomes
NP Polyzos
P-671 Majority of young females with occult POI menstruate regularly: why we should not rely on menstrual status as a marker of ovarian reserve
Y Gűzel
Emerging View to Managing the Poor-Responder
P-468 Cumulative live birth rates after one ART cycle including all subsequent frozen-thaw cycles in 1050 women: RCT comparing GnRH-antagonist versus GnRH-agonist protocol
M Toftager
P-695 The different impact of stimulation duration on oocyte maturation and pregnancy outcome in fresh cycles with GnRH antagonist protocol in poor responders and normal responders
Y-P Li
Special Situations: PCOS and Endometriosis
O-257 The oocyte and embryo quality are poorer in women with endometriosis compared to those without endometriosis
Y Cheong
P-225 The impact of severe endometriosis on embryo quality and pregnancy rate after ICSI
J Sudiman
P-711 High level of androgen during controlled ovarian stimulation cycle impairs endometrium receptivity in PCO patients
D D Wu
Approaches to Hyper-Responsiveness and OHSS
Ovarian hyperstimulation syndrome: a case control study investigating risk factors
S Shields
P-157 Cryopreservation of oocyes for freeze-all policy in women at risk of ovarian hyperstimulation syndrome: preliminary results
P Boyer
Luteal Phase Support
P-720 Luteal phase ovarian stimulation produces competent oocytes in women with diminished ovarian reserve
Z Liu
AFC, AMH and other Biomarkers of IVF Outcome: How Valuable? Biomarker performance in the prediction of ovarian response
A La Marca
P-461 A predictive nomogram based on multiple biomarkers leads to appropriate rFSH starting dose in IVF/ICSI cycles: a randomized controlled trial
A A Marino
This resource is supported by an educational grant from Merck KGaA, Darmstadt, Germany.
Recommended
Management of POSEIDON Groups 3-4
Management of POSEIDON Groups 3-4
ResourcesManagement of POSEIDON Groups 3-4
More Than “Women’s Issues": Women’s Reproductive and Gynaecological Health and Work
More Than “Women’s Issues": Women’s Reproductive and Gynaecological Health and Work
ResourcesMore Than “Women’s Issues": Women’s Reproductive and Gynaecological Health and Work
The Impact of ESHRE 2017 on Japanese Fertility Practice
The Impact of ESHRE 2017 on Japanese Fertility Practice
ResourcesThe Impact of ESHRE 2017 on Japanese Fertility Practice
The Renewed Relevance of Evidence-Based Guidelines for Patient-Centered Infertility Care
The Renewed Relevance of Evidence-Based Guidelines for Patient-Centered Infertility Care
ResourcesThe Renewed Relevance of Evidence-Based Guidelines for Patient-Centered Infertility Care









